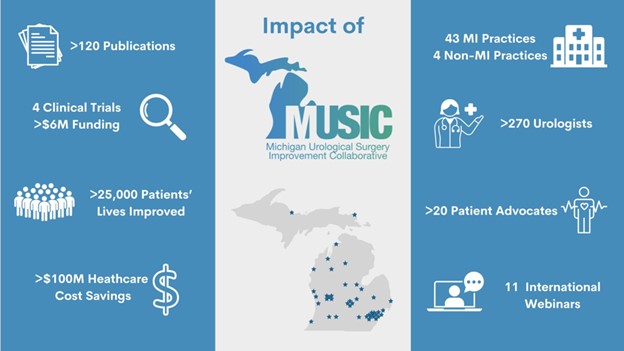
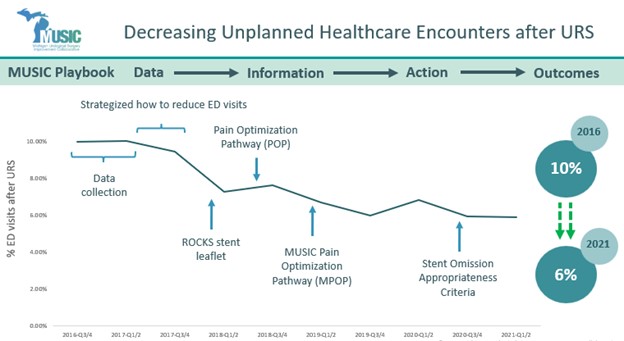
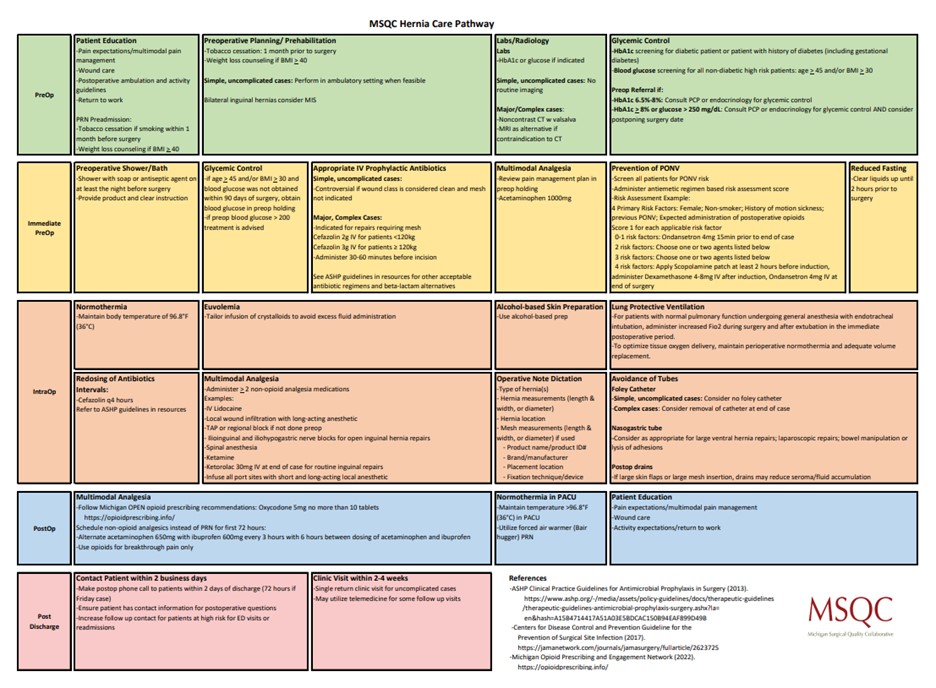
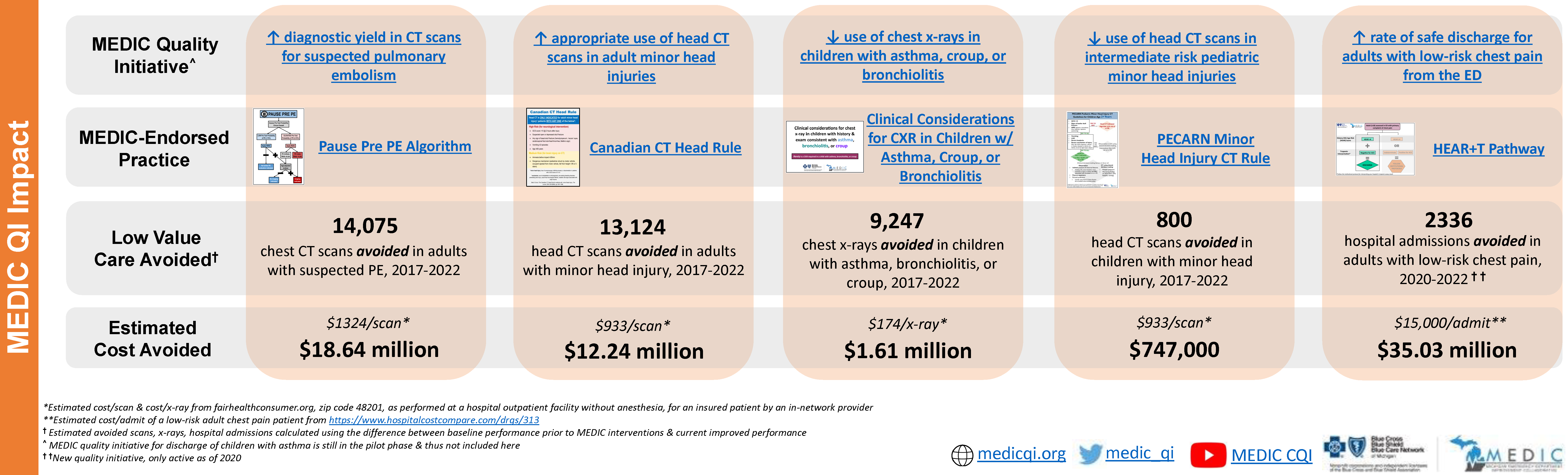
Cancer care is not defined by treatments alone—it is measured by the experiences, quality of life, and outcomes of the people navigating the disease. Across Michigan, patients with cancer face complex clinical decisions alongside challenges that extend beyond the clinic, from treatment side effects to barriers in accessing supportive services. Through statewide collaboration, shared data, and a commitment to improving care delivery, the Michigan Oncology Quality Consortium (MOQC) is working to ensure that patients and their caregivers receive more consistent, compassionate, and high-value cancer care.
Established in 2009, MOQC was tasked with addressing oncology data that showcased significant variation in care outcomes as well as significantly higher costs compared to other areas of healthcare. One of 21 Collaborative Quality Initiatives (CQIs) sponsored by the Blue Cross Blue Shield of Michigan (BCBSM) Value Partnerships Program, MOQC’s aim is to improve access, value, and quality of care for all invasive cancers.
In addition to establishing cross-cutting measures that apply to all disease groups within oncology, MOQC’s work expanded to acknowledge and address the impact of non-medical drivers of health on patient outcomes, intentionally creating space for more patient, caregiver, and frontline voices to shape meaningful change and guide the evolution of cancer care in Michigan.
Services and Benefits for MOQC Members
MOQC provides access to resources and tools, quality improvement initiatives, partnerships, funding, and support that its membership of 54 oncology practices would not otherwise have available. Through collaborative-wide and regional meetings, MOQC fosters member networking, ongoing education on best practices and emerging topics, new publications, and collaboration opportunities. MOQC also meets with oncology practices individually to review their performance measures. For those needing additional support in any area, MOQC conducts root cause analyses in collaboration with the healthcare team and provides resources and consultation on their processes and progress.
Members also benefit from access to the Patient and Caregiver Oncology Quality Council (POQC), a robust and highly engaged patient advocacy group currently comprised of 30 members (Figure 1). POQC gives teams the opportunity to learn directly from the lived experiences of patients and caregivers and brings forward barriers to care that may not be visible in data alone. POQC also contributes to decision-making about quality measures and initiatives through their work on MOQC’s Measures and Steering Committees. Their voices help member practices stay connected to the heart of what they do as they work to help guide MOQC’s efforts toward fair, effective, and compassionate health outcomes across the state (Figure 2).
Figure 1. Patient and Caregiver Oncology Quality Council (POQC)

Figure 2. POQC Member Quote

MOQC members also have the opportunity to establish integrated clinical pharmacist positions providing direct patient care through the Pharmacists Oncology Excellence Program in Michigan (POEM). This program, which has been in place for five years, encompasses 12 pharmacists who support 113 physicians across 28 practices. POEM has been associated with a variety of positive patient care outcomes and clinic time savings relating to clinical care activities.
MOQC’s Key Initiatives and Achievements
Through MOQC’s targeted initiatives, oncology care and outcomes are improving across Michigan. The Palliative Care and Hospice initiative aims to increase time enrolled in hospice to maximize benefits and quality of life for patients and caregivers. By creating tools for how and when to talk to cancer patients about palliative and hospice care (Figure 3), MOQC practices have seen hospice care enrollment improve from 44% in 2017 to 66% in 2024. In the words of a member physician,
“There is so much to help us do better at survival in cancer, and so many more new treatments out there, but the one thing that is often overlooked is – is it the right thing to do for the patient? So I was thrilled to see that MOQC is focusing on hospice. It’s so under looked in oncology these days.”
Figure 3. MOQC Hospice Conversation Guide for Physicians

A complimentary initiative, expanding palliative care access through a partnership with the Center to Advance Palliative Care (CAPC), provides training curriculum to advance practice providers (APPs) regarding primary palliative care, with intentional recruitment in areas of the state that have little-to-no palliative care currently. Those who complete the curriculum attain a certificate from CAPC and integrate primary palliative care into their ongoing care of patients and caregivers.
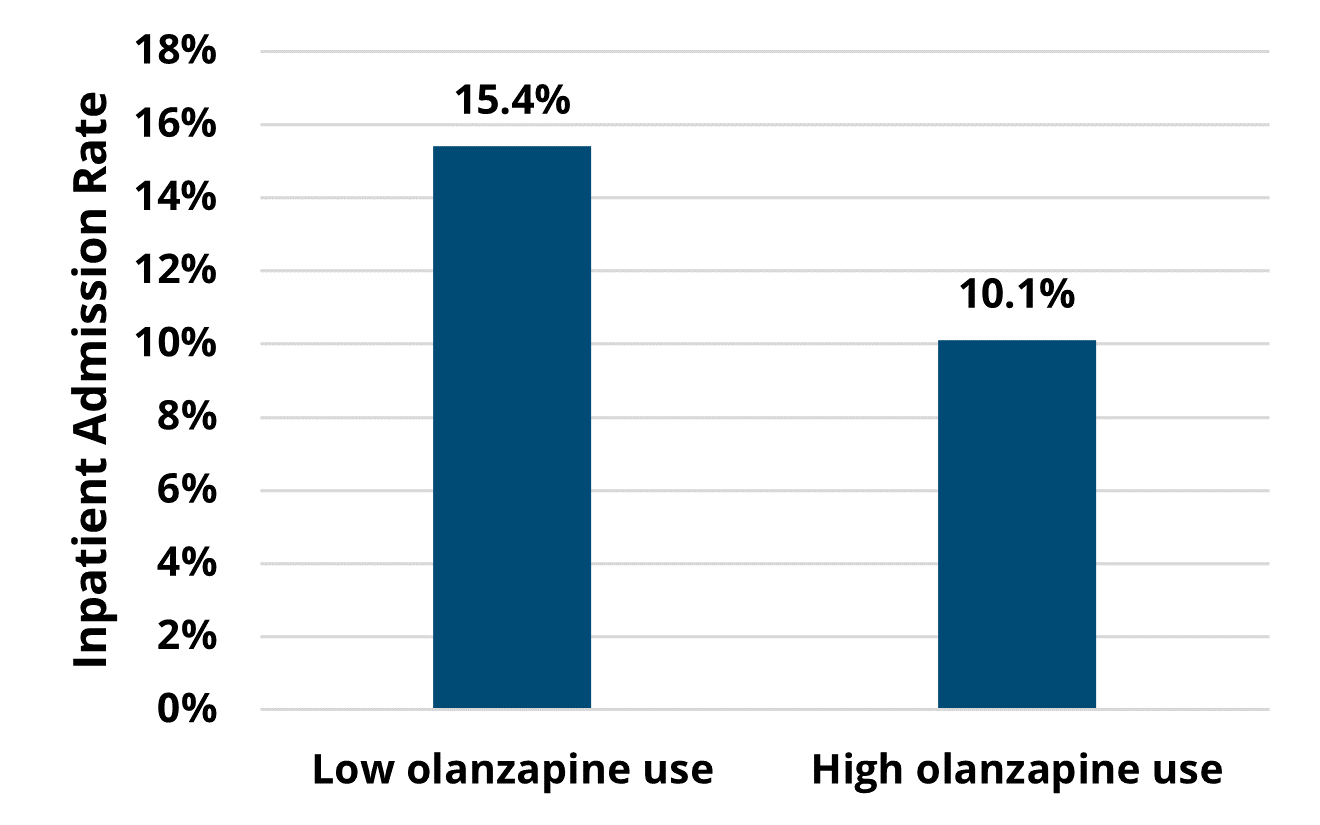
Patient quality of life is an important consideration in cancer care. To address nausea, a common side effect of chemotherapy that significantly impacts patients’ quality of life, MOQC launched a Chemotherapy-Induced Nausea and Vomiting (CINV) – Antiemetics initiative in 2020. The initiative works to increase prescribing of olanzapine to manage treatment-related nausea. Since the initiative began, prescribing of olanzapine has increased from 10% to the notable achievement of 60% in 2024, helping more patients have better treatment experiences. To help evaluate the impact of this effort, MOQC reached out to the Michigan Value Collaborative (MVC) to leverage its robust claims-based data. Together, MVC and MOQC evaluated the impact and value of this initiative in a 2023 impact and value assessment, and the two teams are in the process of refreshing that analysis with newer years of claims data.
Other initiatives include implementing a statewide gynecologic oncology virtual tumor board to support multidisciplinary learning, standardize care recommendations across practices, expand access to clinical trials, and expand perspectives for clinicians caring for patients throughout Michigan. MOQC helps optimize statewide treatment of advanced non-small cell lung cancer via an oncology stewardship initiative focused on improving biomarker testing across the state and increasing education around targeted therapies.
In addition to centering patient voices through POQC and many other MOQC accomplishments, a major achievement of MOQC is the development of a comprehensive Excellence in Quality Certification program that recognizes oncology practices providing high-quality and high-value care. Eligibility criteria include a site visit to ensure safe practices regarding anticancer therapy, measure performance, medical record review, and policy review. All criteria measure policy and practice to validate that oncology care is guideline-concordant and recognizes substantial decreases in variations in care and in costs of care (Figure 4). A key component of the certification is creating an action plan to close non-medical gaps in healthcare, ensuring all cancer patients in Michigan have the same access to high quality care. Fourteen out of MOQC’s 54 practices were certified in 2024, and 23 practices pursued certification in 2025.
Figure 4. MOQC Excellence in Quality Certification Criteria

MOQC is proud of its commitment to addressing the non-medical needs of patients and caregivers through the POQC and the Excellence in Quality Certification program. Additional ways MOQC centers this aspect of patient care is by endeavoring to provide patients with increased access to supportive services and resources, including standardizing screening for non-medical needs, integrating referrals to Michigan 2-1-1 into electronic medical records (EMR), providing meals to patients who are currently food insecure and receiving anticancer therapy (plus up to one caregiver per patient), and facilitating financial navigation training for interprofessional members of oncology care teams. Non-medical patient needs and gaps in care are also being addressed through MOQC’s stewardship initiative, which aims to improve the use of systemic anticancer therapy with the goal of enhancing patient health outcomes while reducing financial strain on patients. In addition, MOQC conducts multivariate analyses of its measures annually to find gaps in care based on demographic categories. These analyses allow MOQC to review variation among practices and collaborate individually with them as needed to close gaps.
Looking Ahead: Continuing to Drive Whole Team Collaboration
MOQC’s work offers a reminder that improving oncology care often requires thinking beyond traditional approaches. By weaving patient and caregiver experiences into the fabric of their work, MOQC is able to look for gaps in care, prompt new questions, and reshape how they understand quality. MOQC’s initiatives and learning opportunities (such as interprofessional development sessions, the statewide tumor board, the palliative care certificate program, and addressing non-medical needs) are shaped with recognition that there is a whole team involved in the patient care related to MOQC’s quality measures. MOQC invites practices to engage with quality improvement in ways that expand perspective and challenge existing healthcare power dynamics. Through this multifaceted approach, MOQC is always striving to look for a deeper partnership with all of the people most affected by the outcomes.
The BCBSM-funded CQIs play a crucial role in driving healthcare quality improvement in Michigan. MVC is excited to continue highlighting the innovative contributions of individual CQIs and the ways in which MVC’s data are supporting high-value care initiatives across the portfolio. Please reach out to MVC by email if you are interested in learning more.