In February, MVC hosted its first virtual networking event of 2026 with a special presentation on relational coordination by MVC Project Manager Emily Woltmann, PhD, MSW, and Richard Wylde, MSc, Deputy Director of Improvement at Leeds and York Partnership, National Health Service (NHS) Foundation Trust. With more than 45 attendees, the event introduced members to relational coordination, a framework that can be used to evaluate and strengthen collaboration and teamwork in healthcare settings. Following presentations, participants joined breakout groups to discuss the content and complete a case study activity, followed by a debrief and wrap up discussion.
Overview of Relational Coordination
Woltmann kicked off the event with an introduction to relational coordination, which was first introduced by Jody Hoffer Gittell as a mutually reinforcing process of communicating and relating for the purpose of task integration. She introduced participants to the relational coordination framework developed by Braneis University’s Relational Coordination Collaborative (RCC), which showcases how relationships and communication continuously reinforce each other in positive and negative ways. In relational coordination, the main components being considered are whether communication that occurs is happening in a frequent, timely, and accurate manner and is being used with the intention of problem-solving; while relational components reference shared goals and knowledge rooted in mutual respect.
Relational coordination is a dynamic theory, where many areas influence each other. In addition to communication and relational components, the full framework (Figure 1) describes the types of structural, relational, and work process interventions that may impact communication and relationships to impact downstream outcomes.
Figure 1. RCC’s Dynamic Theory of Coordination

Structural interventions are implemented by leadership roles and include things like shared meetings, huddles, information systems, and boundary spanner roles that cross over multiple departments. Relational interventions focus on directly improving ways people relate to each other, such as cultivating safe spaces for discussion. Finally, work process interventions focus on workflows and sometimes use plan, do, study, act (PDSA) cycles for improvement.
Woltmann highlighted some of the methods available for measuring relational coordination, including a validated quantitative survey to measure role-based coordination between team members. The survey can help evaluate how well relational coordination is working between different roles. Another measurement tool that can be used is relational coordination mapping (Figure 2), which is a visual way to view responses from the relational coordination survey and summarize the strength of relationships between groups. It is designed to encourage deeper engagement and reflection among participants.
Figure 2. Measuring Relational Coordination: Relational Coordination Mapping
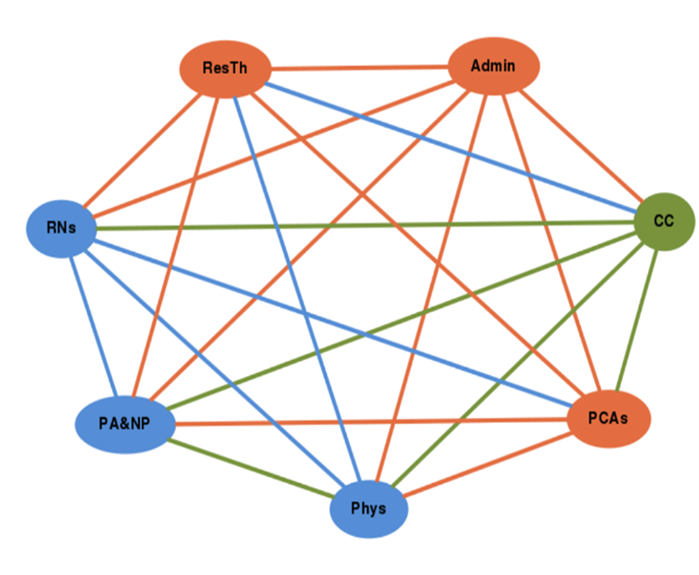
Woltmann explained that when relational coordination is working well and is strong, it supports organizations in achieving a wide range of desired performance outcomes such as quality, safety, efficiency, staff well-being, learning, and innovation.
The Maryland and Michigan DECIPHeR Project - Relational Coordination in Community Mental Health Settings
Woltmann also discussed lessons and insights she gleaned about relational coordination from the Maryland and Michigan DECIPHeR Project, which focuses on implementing interventions that decrease cardiovascular disease (CVD) risk factors in people with serious mental illness. Led by Dr. Amy Kilbourne, PhD, MPH, in the Department of Learning Health Sciences at the University of Michigan, and Dr. Gail Daumit, MD, MHS, at Johns Hopkins University, the project focuses on identifying effective interventions shown to address CVD risk factors in persons with a serious mental illness. This broader implementation trial is researching ways to implement a new intervention called IDEAL GOALS in behavioral health homes (BHHs).
While analyzing the qualitative data for this needs assessment phase of the project, Woltmann and colleagues became interested in using relational coordination to understand relational aspects of care coordination in the BHH context. The sample for this study included 14 sites across Michigan and Maryland, with 14 nurses and 32 frontline staff. Sites were given a qualitative designation of “consistently positive” relational coordination, “consistently negative” relational coordination, or “mixed” relational coordination.
Of the 14 sites, Woltmann said five had a consistently positive relational coordination level, six had a consistently negative level, and three had a mixed result. The research team found that sites with consistently positive relational coordination had a variety of structural factors in place to support RC. Boundary spanner roles were seen as particularly important in achieving good relational coordination, as they take on the role that crosses the gap in care for patients – in this instance community mental health staff to primary care providers. Results from the study indicated there were many kinds of strategies that sites used to develop functional RC, and that the most imperative component to building positive relationships was having a strong sense of trust.
Relational Coordination in Mental Health Services – The National Health System
Following Woltmann’s presentation, Richard Wylde, Deputy Director of LYPFT, provided participants with an in-depth look at how relational coordination is being utilized in his work at the National Health System (NHS) of England and emphasized how important coordination is in a large healthcare system. The NHS employs 1.5 million staff to care for roughly 1.7 million patients daily. With a tax funded healthcare model, each patient’s care is financially covered (£188 Billion per year) (Figure 3).
Figure 3. The English NHS in Numbers and Why Improvement Matters
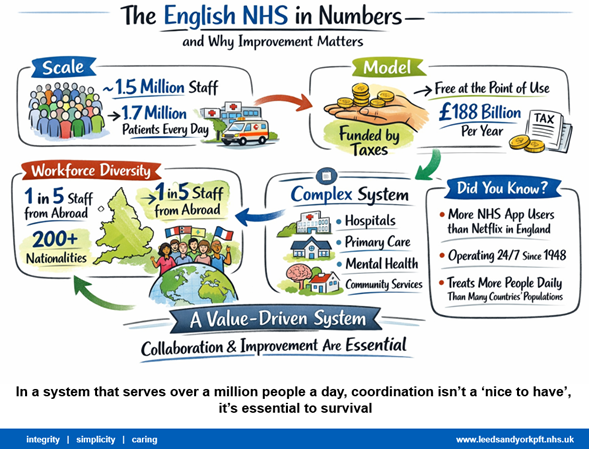
The NHS has a complex system of hospitals, primary care clinics, mental health clinics, and community services. Wylde is a part of the Leeds and York Partnership NHS Foundation Trust (LYPFT) which provides specialist mental health and learning disability services to the people in Leeds West Yorkshire, England. They have 48 locations, including 408 beds, see over 25,000 new patients, and have contact with over 270,000 people in the community per year.
Wylde shared that the NHS relationship coordination journey began with senior leadership who had previous experience with relational coordination, introducing the concept and promoting it to other leaders and the board. He recounted that there was slow organizational uptake of relational coordination theory within the system initially. However, as other leadership saw the benefits, they were able to implement strategies at other organizational levels.
Within the community mental health services system, the LYPFT program wanted to look at how young people transition to adult mental health services. They found that it was important to provide a safe space for players in the system to come together to better coordinate this process, and to be mindful of the many different perspectives and power imbalances present. One of the barriers they experienced, Wylde said, was the difficulty in balancing the need for human relationships and trust building timelines versus the systems' need for quick answers.
Wyle highlighted several key lessons learned through implementing relational coordination at multiple levels of a system, including:
- Governance at the board level can have limitations on time for developing a relational space
- Relational coordination worked best when senior leaders had a collectively shared understanding of what relational coordination was and how they could use it
- Relational coordination was more successful when it had clear framing and context to the program/service/team
- It was important for all levels to understand how the relational coordination dynamic functions at the smallest level of a system (between people)
- Relational coordination is both a relationship and a process
- Strong relationships enable strong processes and vice versa
Breakout Session Debrief
During the breakout session portion of the networking event, participants were guided through a patient case study that demonstrated how breakdowns in staff communication and relationships could negatively impact patient outcomes. The breakout groups had engaging conversations that focused on building trust, relational coordination interventions, explaining the “why” to help teams develop shared goals, understanding the impact of staff-to-patient ratios on communication, and other tools and frameworks that have helped teams improve their communication.
MVC was glad to highlight this topic and the expertise of these presenters to support shared learning and continuous improvement within healthcare teams. MVC welcomes presenters to share their expertise, success stories, initiatives, and solution-focused ideas with MVC members, which cultivates a community of peers looking to collaborate in a non-competitive space. Please reach out to MVC by email if you are interested in being a presenter or submit a presentation proposal online.