Health equity has captured the attention of healthcare. It was a top trend for healthcare providers in 2021, and surveys indicate it will be one of the main priorities for large healthcare employers in 2022. It is also a key strategic focus of the MVC Coordinating Center in the years ahead. As such, MVC is building out offerings for its members in this space, which began with the launch of its new health equity report and was followed by a semi-annual meeting dedicated to the topic in October 2021. Most recently, MVC launched a new health equity workgroup, which will continue to meet on a bimonthly basis in 2022.
The first health equity workgroup took place this week featuring speakers from the MSHIELD (Michigan Social Health Interventions to Eliminate Disparities) collaborative—one of the newer teams in the Blue Cross Blue Shield of Michigan Collaborative Quality Initiative (CQI) portfolio. MSHIELD Co-Director Dr. John Scott co-presented with MSHIELD Program Manager Carol Gray. They were joined by 72 attendees representing hospital teams, physician organizations, fellow CQIs, and other areas. The presentation focused on the role of MSHIELD in addressing social risk factors in healthcare as well as members’ approaches to health needs screening, referral, and linkage.
The social determinants of health (SDOH) have a tremendous impact on patient health outcomes, resulting in Healthy People 2030 naming it one of its five priorities. With thousands of journal articles confirming the impact of the SDOH, there is now a shared understanding across healthcare providers that this area is a priority. In fact, it affects patient health outcomes significantly more than clinical care (see Figure 1). MSHIELD’s presenters highlighted this fact and used it as an opportunity to define a common language for the discussion. They said health equity is achieved when every person can attain their full health potential and no one is disadvantaged from achieving this because of socially determined circumstances.
MSHIELD will serve as a link between the healthcare system, the community resources that can reliably serve patients’ social needs, and the communities that are home to those patients. To that end, MSHIELD will help establish partnerships with key healthcare and community entities and promote the exchange of data and services in a way that helps achieve health equity.
Unlike some of the “legacy” CQIs that are clinically focused, MSHIELD will fill a consulting role with other CQIs to help them set and meet goals related to health behaviors and social needs. Since health equity is a multi-faceted issue affecting all areas of health, MSHIELD also has an unlimited population and practice focus. For the time being, however, the speakers identified that MSHIELD is particularly interested in food access, housing instability, and transportation since those are areas with the strongest evidence for impact in a clinical setting.
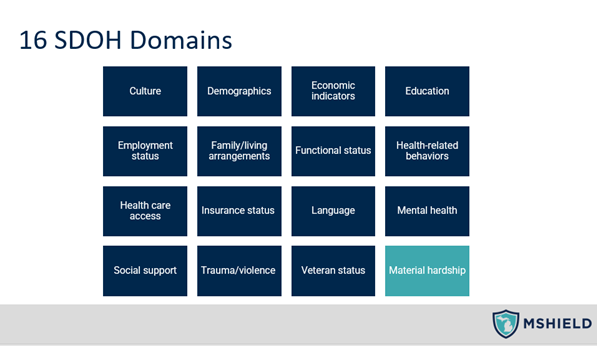
MSHIELD’s presenters also summarized their findings from an environmental scan of the larger CQI portfolio. Last year they surveyed the other CQIs in the BCBSM Value Partnerships portfolio to identify what types of SDOH data they may collect and how. Of the 16 SDOH domains (see Figure 2), MSHIELD found that almost all CQIs collect data on demographics, insurance status, and health-related behaviors. However, only three CQIs currently collect data related to material hardship (e.g., food insecurity, housing insecurity, transportation, medication affordability, access to technology, childcare, etc.). MSHIELD hopes to help build on what has been collected so far and assist providers and CQIs alike in their pursuit of health equity initiatives.
Figure 2. Domains of the Social Determinants of Health from MSHIELD Presentation
The workgroup concluded with an active discussion about current practices and challenges experienced by providers in identifying, referring, linking, and following up with patients. Representatives from physician organizations and hospitals alike shared examples about how they integrate screening and capture this data, which led to conversations about the technologies used to assist with this process and the value of universal versus targeted screening strategies. Most of the participants who shared their experience expressed that whichever strategy they adopted, there were efforts to make the screening questions accessible for those with language or literacy barriers. Examples of this that were provided by members included translating materials to common languages from their local community and utilizing the professional abilities of social workers on site. There were also discussions about how to best identify resources within a given community for the purposes of referrals, with some thoughtful suggestions about partnering with community health needs assessment teams and social workers from within hospitals.
To hear the full discussion and learn more details about MSHIELD, the full recorded workgroup can be viewed here. MVC looks forward to continuing this health equity conversation on March 16. Register for the next MVC health equity workgroup here. If you would like to receive future MVC workgroup invitations or you have an idea for a future speaker, please contact the Coordinating Center at michiganvaluecollaborative@gmail.com.
Speaker Biographies:
Dr. Scott is an Assistant Professor of Surgery in the Division of Acute Care Surgery at the University of Michigan. His health policy and health services research interests are focused on improving access to timely, affordable, high-quality surgical care for the acutely ill and injured.
Carol Gray leads the overall management, performance, and coordination of the MSHIELD program and team. She has extensive experience managing public health research teams, communicating across and coordinating with multiple partnerships, and linking and engaging with community-based organizations.




