As hospitals begin to identify lessons learned since the start of the pandemic, providers are keenly aware of the prevalence and exacerbation of existing health inequities. Despite the fact that many providers are increasingly interested in addressing the social determinants of health (SDOH) and equitable access to care, communities of color and other minorities that are statistically more impacted by SDOH and socioeconomic status (SES) have endured even wider gaps in health outcomes and care this past year. For many hospitals and physician organizations, the way forward requires the application of a health equity or social risk lens across the board, so that basic healthcare and quality improvement decision-making can be maximized for all patient populations, not just those with fewer social risk factors. The MVC Coordinating Center is, therefore, proud to have released its first MVC Health Equity Report to its membership on Wednesday morning.
MVC began developing metrics for its membership in this area over the past year so providers might better understand where inequities are materializing within the four walls of their hospitals and beyond. One popular method for identifying low-SES patients is by determining where someone lives and applying population-level metrics to the individual. Examples of this would be using the Area Deprivation Index (ADI) or Social Vulnerability Index (SVI). Both indexes are based on census tract data and provide SES characteristics about a population within a specific geographic location (i.e., a census tract), including risk factors such as poverty, education level, transportation access, and housing security. However, in developing the MVC Health Equity Report, the MVC Coordinating Center elected to utilize a patient-level metric of SES that is compatible with MVC claims data. As a result, the report identifies low-SES patients using dual-eligibility status.
Dual-eligible beneficiaries are patients that are eligible for both Medicare and Medicaid. In the MVC Health Equity Report, dual eligibility is defined as having been eligible for both Medicare and Medicaid at any point during the year of the index admission and is limited to patients that were at least 65 years old at the time of admission. Medicaid eligibility is a good indicator of SES when using claims data since it is income-based, and studies have shown that there is a strong association between low-income status and adverse health outcomes. Dual eligibility allows MVC analysts to identify Medicaid-eligible patients within its more extensive Medicare data set for analyses. Medicare data on the MVC registry currently includes claims data from 1/1/2015 through 9/30/2020. The resulting reports prepared for members focuses on episodes occurring between 2017 and 2020, or between 2017 and 2019 if the circumstances of 2020 resulted in unusual case counts by facility.
In developing this report, there was a conscious decision to exclude any sort of comparison group alongside each individual hospital's metrics. This is because the socioeconomic factors of a hospital’s patient population cannot be changed, and there is great diversity between hospitals throughout the state and within geographic regions. For those reasons, benchmarking was not the intention of this report. However, it is important to note that across the state, the data analyzed by the MVC Coordinating Center consistently indicates that dual-eligible patients have poorer outcomes than their non-dual-eligible counterparts, including longer lengths of stay, higher readmission rates, higher post-discharge emergency department utilization, lower rates of office visits post-discharge, higher rates of post-discharge outpatient procedures, and higher utilization of skilled nursing facilities. Blinded sample graphs for length of stay (Figure 1) and readmission rates (Figure 2) were created using data from three distinct, large hospitals in order to showcase some of these differences.
Figure 1.
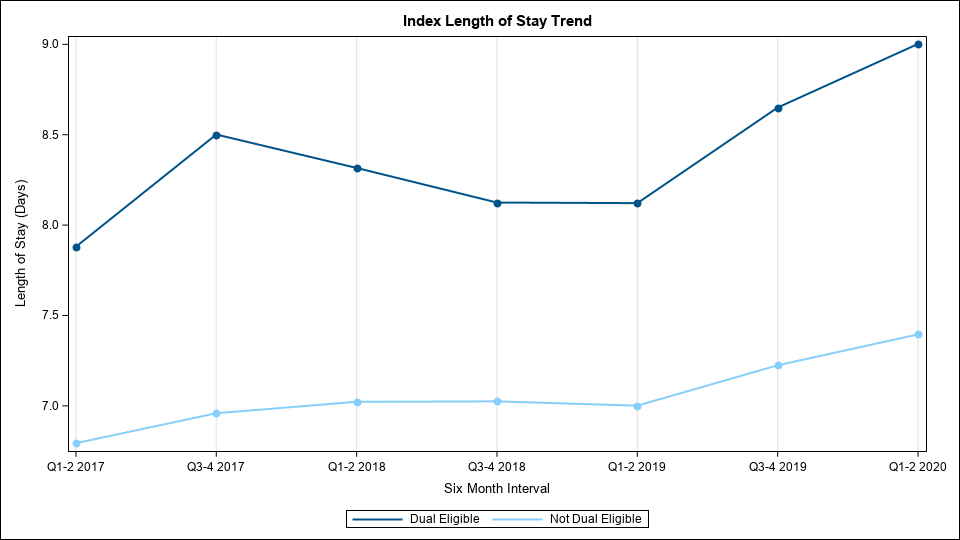
Figure 2.
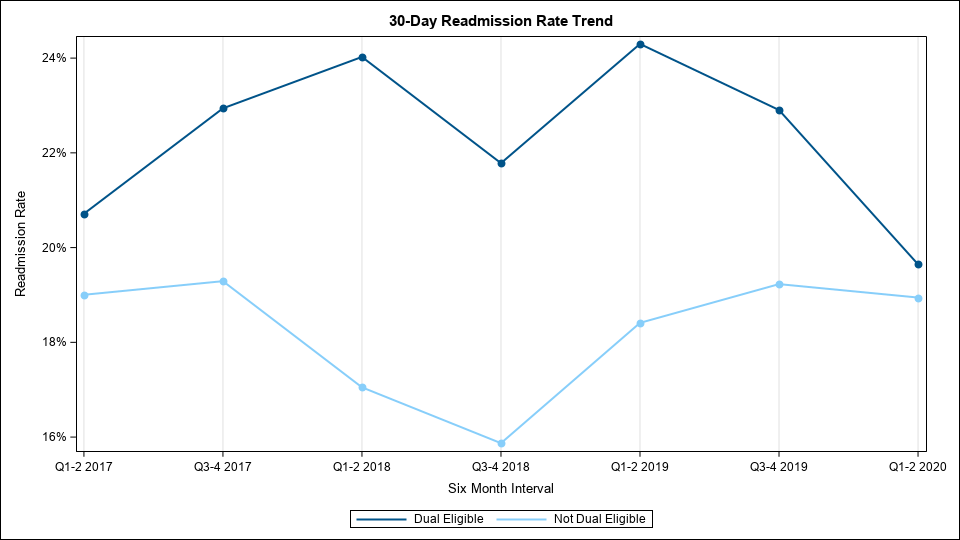
Members receiving reports will see a variety of graphs depicting, for example, total episode payment trends, 30-day readmission rate trends, and post-acute care utilization. Also provided is a table outlining a hospital or region’s highest volume of conditions within its dual-eligible population (see Figure 3 for a blinded sample). The purpose of this table is to help members better understand the proportion of dual-eligible patients at their hospital and the prevalence of various conditions within that population. It will also help members to better understand their report overall by identifying the conditions and procedures driving the various metrics included within it.
Figure 3.
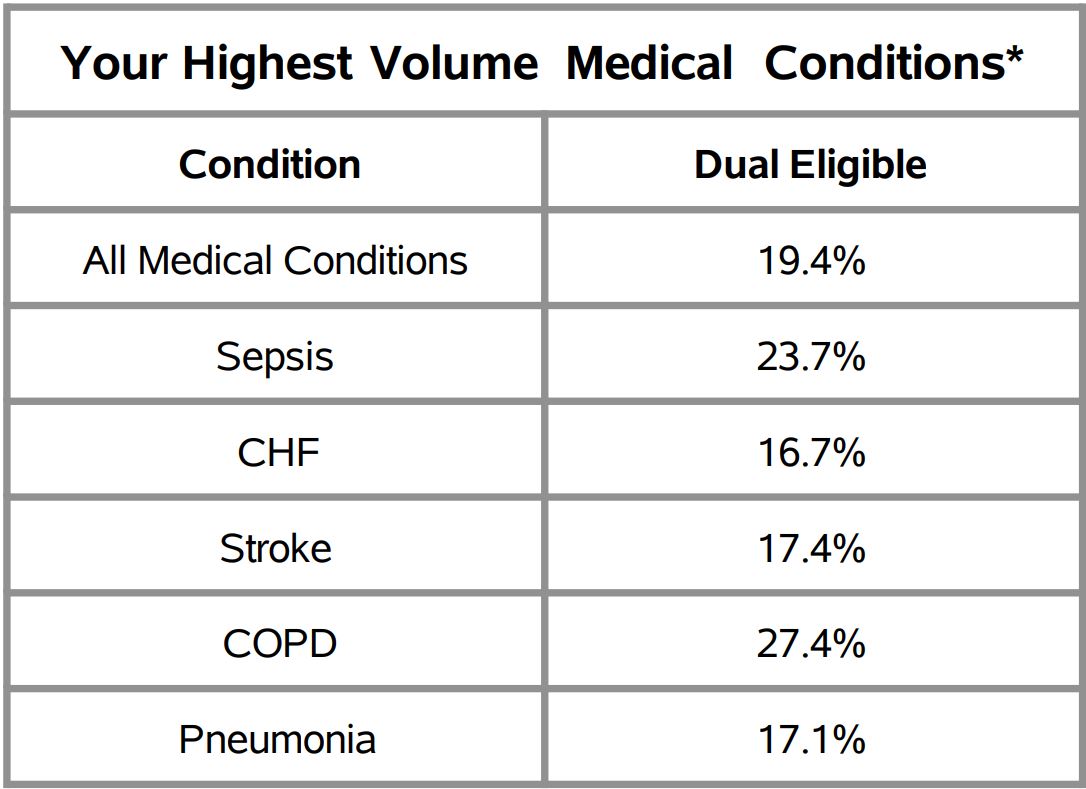
MVC is eager to do more in this space in the months ahead. With the recently added Michigan Medicaid data on the MVC registry, the Coordinating Center has a new opportunity to more closely examine the types of disparities that are prevalent in healthcare. Additionally, with the addition of 13 rural or critical access hospitals to the collaborative in the past 12 months, the Coordinating Center aims to expand its metrics outside of the episode structure to examine population health metrics. This will allow for better understanding about healthcare delivery and how outcomes differ in rural regions compared to urban.
The MVC Coordinating Center wants to hear feedback from its members. With the addition of Medicaid data, we are working hard to develop more metrics and reports that focus on health equity. If you have any questions, comments, or suggestions, please contact the MVC Coordinating Center at michiganvaluecollabortative@gmail.com.



