The MVC Coordinating Center recently distributed its first-ever report based on new emergency department-based episodes (“ED-based episodes”), sharing versions with site coordinators and quality improvement staff at 102 participating MVC member hospitals across Michigan. Reports featured each hospital’s own attributed ED-based episode data for five high-volume ED conditions: chest pain, abdominal pain, chronic obstructive pulmonary disease (COPD), congestive heart failure (CHF), and cellulitis.
ED-based episodes are a new episode of care data structure developed this past year by MVC in collaboration with the Michigan Emergency Department Improvement Collaborative (MEDIC), a BCBSM-funded Collaborative Quality Initiative with the goal of improving care and patient outcomes in Michigan emergency departments. MVC and MEDIC team members worked closely to develop 30-day episodes of care initialized by a patient’s visit to the ED and including all claims-documented care received in the 30 days following a patient’s index ED visit. MEDIC program director Dr. Keith Kocher, MD, talks more about the collaboration as well as advice on leveraging this data from an emergency medicine perspective in the video below.
These ED-based episodes are built using medical claims data from Medicare Fee-for-Service, Blue Cross Blue Shield of Michigan PPO Commercial and Medicare Advantage plans, and Blue Care Network HMO Commercial and Medicare Advantage plans. MVC’s ED-based episodes of care include both adult and pediatric patients, providing new opportunities for quality improvement insights at Michigan hospitals. Though this report provides metrics for five specific index conditions, MVC currently offers data for 15 ED-based index conditions, including abdominal pain, asthma, atrial fibrillation, cellulitis, unspecified chest pain, COPD, CHF, deep venous thrombosis, diabetes mellitus (short- and long-term complications), gastrointestinal bleed, pneumonia, pulmonary embolism, pyelonephritis/urinary tract infections, and syncope.
For each of the five index conditions included in the recent reports, hospitals received information on risk-adjusted and price-standardized 30-day total episode payments, same-day inpatient admission rates over time, utilization of healthcare services across the patient’s 30-day episode of care, and each hospital’s most frequent reasons for inpatient readmissions. Patient claims data were included for adult patients aged 18 and older who had an ED visit at a given hospital between 1/1/21 and 8/31/22, were insured by one of the insurance plans mentioned above, and had a primary diagnosis on their index claim matching standardized definitions for the five included conditions.
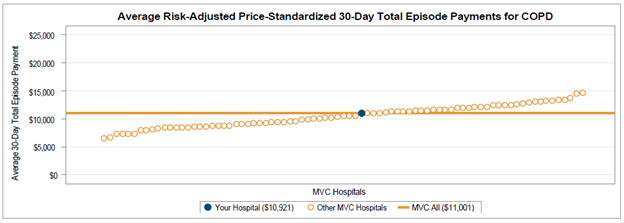
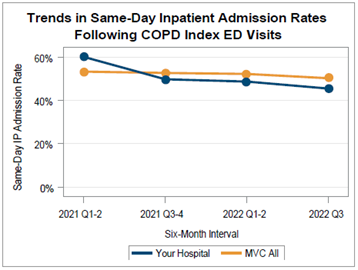
Among general acute care hospitals receiving a report, the average risk-adjusted, price-standardized 30-day total episode payments (Figure 1) for the five reported conditions were highest for CHF ED-based episodes ($17,455) followed by COPD ED-based episodes ($11,001), and lowest for unspecified chest pain ($3,792). Within each condition, MVC 30-day total episode payments were consistently higher for episodes in which the patient had a same-day inpatient admission compared to episodes in which the patient did not have an inpatient stay begin on the date of their ED visit. With that information in mind, hospital members can also use their individualized reports to track their same-day inpatient admission rate by six-month intervals using trend graphs for each included ED-based condition (Figure 2).
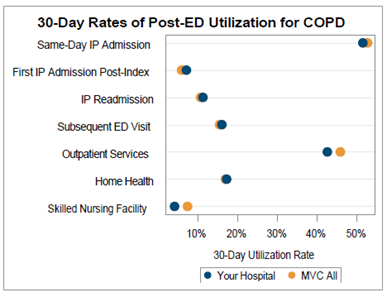
A key goal for these ED-based episode reports was to provide insight into healthcare utilization following index ED visits. Therefore, reports included a dot plot (Figure 3) comparing their own hospital’s patient post-ED utilization to that of the appropriate general acute care hospital or Critical Access Hospital MVC comparison group. Dot plots provided information on what percent of episodes had a same-day inpatient admission, what percent did not have a same-day inpatient admission but did see the patient admitted in the 1 to 30 days following the index ED visit, and what percent of patients had two or more inpatient admissions (thus, at least one readmission) during the episode of care. Also provided are rates of subsequent ED visits, receipt of outpatient services, home health, and skilled nursing facility care.
Please share your feedback with the MVC team if certain report measures were helpful or if you’d be interested in seeing future ED-based episode reporting for certain conditions and metrics. MVC is now also accepting custom report requests using its new ED-based data. Contact MVC to learn more.