This week the Michigan Value Collaborative (MVC) distributed mid-year scorecards for Program Year (PY) 2023 of the MVC Component of the Blue Cross Blue Shield of Michigan (BCBSM) Pay-for-Performance (P4P) Program. PY2023 scores achievement and improvement points for each hospital’s selected episode spending conditions using index admissions from 2022 as the performance year against admissions in 2020 as the baseline year. Hospitals can earn up to five points for each condition using the higher of a hospital's achievement and improvement point scores. This is the second year of a two-year (PY22-23) P4P cycle.
This cycle also offers hospitals bonus points for completing and submitting a survey for each selected condition by November 15, 2022. These surveys will be used by the MVC Coordinating Center to improve the program for future years and support practice sharing between members. The full methodology for this program cycle can be found in the PY2022-2023 Technical Document.
Figure 1 below illustrates the current distribution of total hospital points out of 10. The average points scored across the mid-year scorecards was 6.4/10 before including the survey bonus points. This is 0.4 points higher than the average points scored at the conclusion of PY22 excluding all bonus points.
Figure 1.
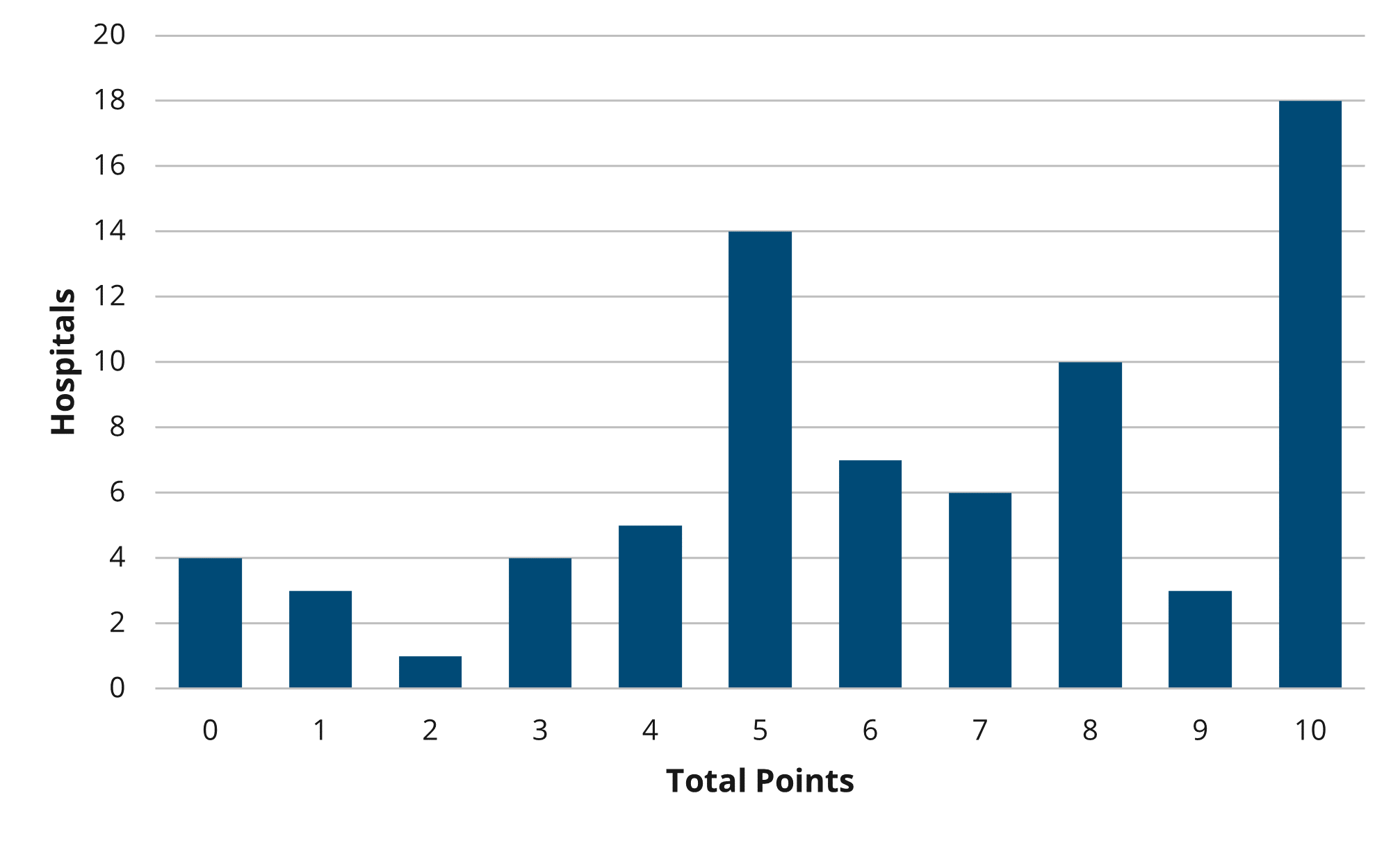
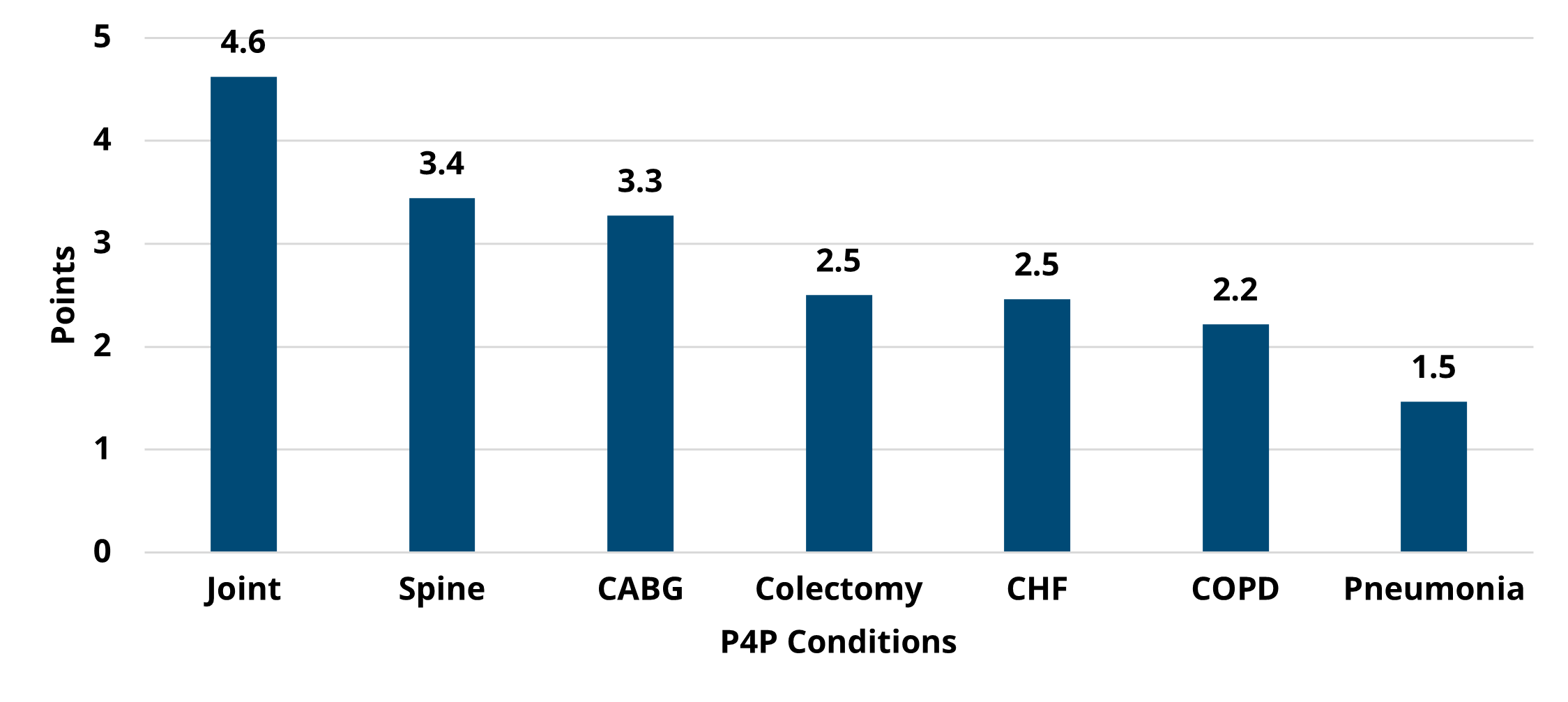
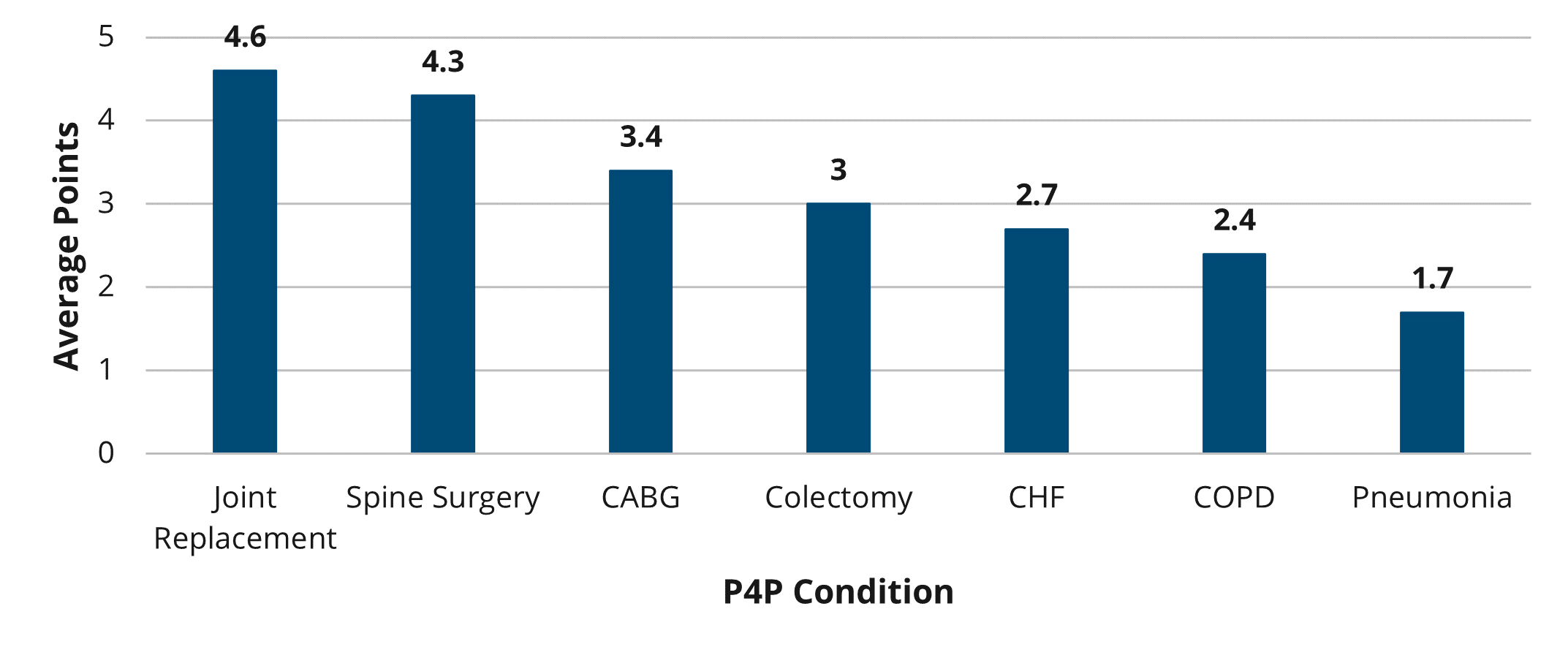
Figure 2 below illustrates the breakdown of average points by condition. Hospitals could earn up to five points for each condition. Consistent with previous years, joint replacement was the highest scoring condition with an average of 4.6 points. Much of the success observed for the joint replacement condition can be attributed to the shift from post-acute care in skilled nursing facilities (SNF) to home health and the move towards outpatient surgeries. Pneumonia was the lowest scoring condition with hospitals earning less than two points on average.
Figure 2.
These mid-year P4P scores are subject to change as new data is added. The final scorecards will be distributed after all 2022 claims are incorporated. Hospitals can track their score through the P4P PY22-23 reports on the MVC registry, which provides all relevant scoring information for both improvement and achievement points in one place (bonus points are not reflected on the registry). These registry reports can be filtered by selected conditions to make the tracking of P4P points easier. Contact the MVC Coordinating Center for a walkthrough of your hospital’s PY23 mid-year scorecard or P4P registry reports.