Today the MVC Coordinating Center published its annual Qualified Entity Certification Program (QECP) public report for 2023. One of the requirements of being a qualified entity (QE) with the Centers for Medicare & Medicaid Services (CMS) through the QECP is the annual dissemination of a public report created using claims data. MVC shared its first public report last year, making the 2023 report the second iteration.
As with last year, the 2023 MVC QECP Public Report provides unidentified aggregated data on Michigan hospitals for two measures: rates of 30-day rehospitalizations following start of home health care, and rates of outpatient follow-up received after hospitalization for congestive heart failure (CHF) or chronic obstructive pulmonary disease (COPD). Both measures were created using data from episodes of care initialized by inpatient hospitalizations or surgeries between 1/1/2018 and 12/31/2021.
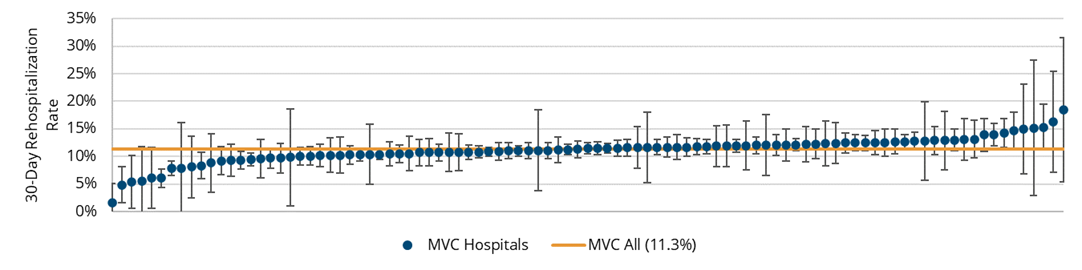
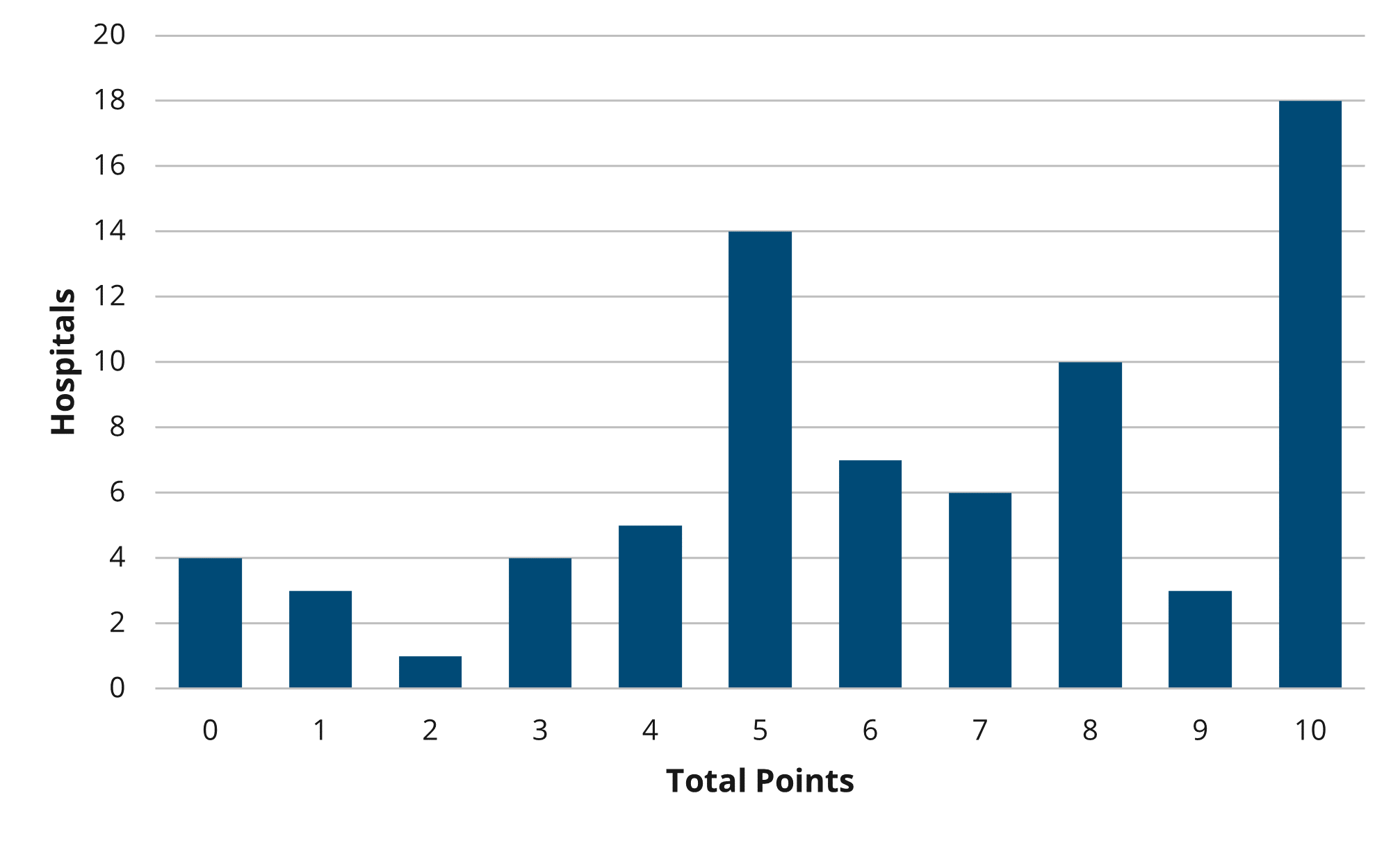
For 2018-2021, the overall rate of 30-day unplanned rehospitalizations from home health among MVC member hospitals in Michigan was 11.3%. Risk-adjusted rates by index hospital ranged from 1.6% to 18.5% (Figure 1). By home health provider, risk-adjusted rates ranged from 2.0% to 23.6%. Patients whose episode of care began with an index event for endocarditis, COPD, CHF, or percutaneous coronary intervention (PCI) were more likely than patients with other index conditions to experience an unplanned rehospitalization in the 30 days after they started home health care.
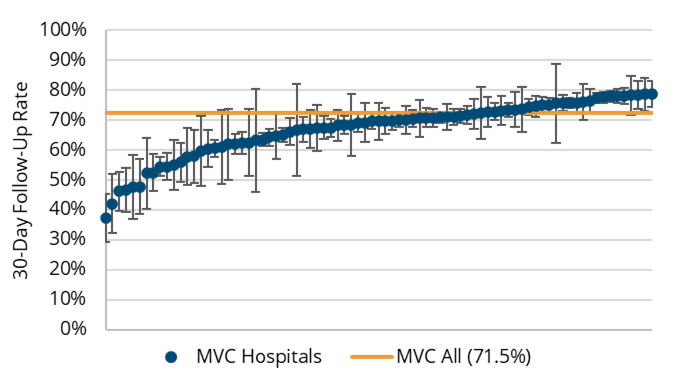
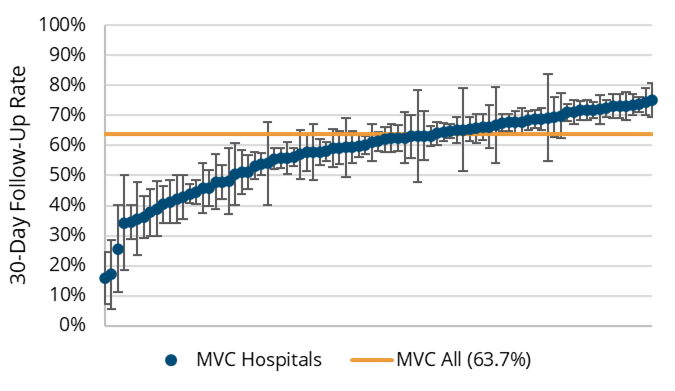
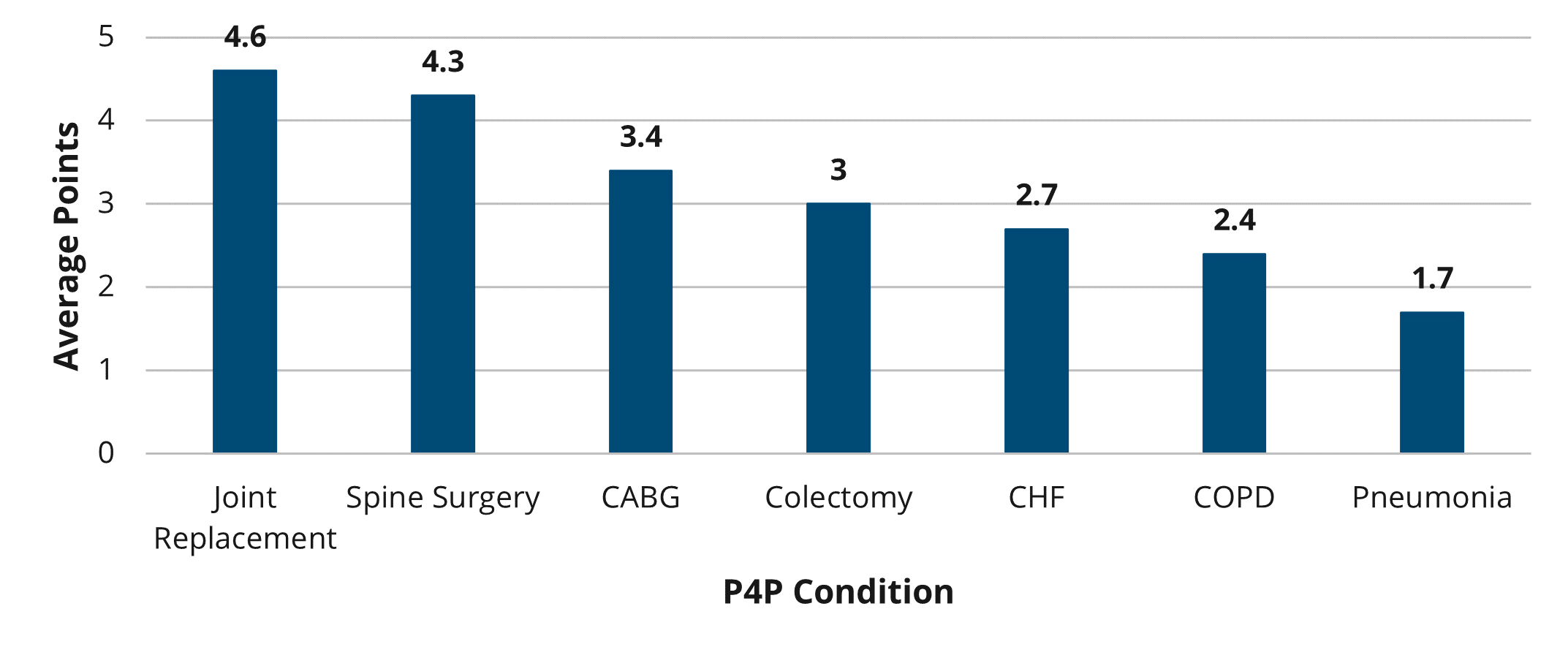
Across the 102 MVC hospitals with attributed episodes of care data underlying this report, the unadjusted rates of patients receiving outpatient follow-up were higher following index hospitalizations for CHF than for COPD (Figures 2 and 3). This was the case whether follow-up occurred three days (16% vs. 13%), seven days (45% vs. 37%), 14 days (63% vs. 54%), or 30 days (72% vs. 64%) after discharge.
For more information and the entire set of findings, we invite you to read the full report, which is available online to any member of the public on the MVC Resources page or directly here.
QE certification status allows MVC to provide hospital members with additional data from Medicare Fee-for-Service (FFS) claims at a level of granularity not otherwise available under standard CMS data use agreements. Reports located under the “QE Data” icon on the MVC registry allow hospital registry users to see unsuppressed data that include case counts <11 as well as utilization rates and average payments based on case counts <11. In addition, on any QE Data registry report, members can click on specific data points to load a list of all episodes underlying that data point. From that episode list, it is possible to view drill-down information on any individual listed episode to learn more about the claims and price-standardized payments comprising that episode.
MVC members representing one or more MVC-participating hospitals can send an email to Michigan-Value-Collaborative@med.umich.edu to learn more about data available through MVC’s QECP reports and to receive the forms necessary to gain access to those registry reports.