In recent years, the pursuit of high-quality healthcare has pushed an increasing number of organizations to consider how tailored approaches can reduce variation in health outcomes, increase the value of care, and enhance patient experiences with the healthcare system. Reflecting this growing recognition, the Michigan Value Collaborative (MVC) surveyed its members in 2024 to better understand how members were identifying gaps in care and responding to non-medical drivers of health. With questions focused on data collection, strategic planning, and programming, MVC gleaned a wealth of impactful and innovative solutions already under way in hospitals across the state.
For the majority of the surveyed hospitals, the most common focus areas for programming were enhancing provider availabilitiy (i.e., telehealth, mobile units, and nontraditional clinic hours), improving access to reliable transportation, offering financial support, and providing translated materials. Although it is common for hospitals to have strategies in place in these areas, the specific approaches are often as varied as the communities they serve.
At Marshfield Medical Center-Dickinson, for example, one way they approach gaps in preventative care within the community is through dental care programming. Recent studies have established a clear link between oral health and overall health, underscoring the importance of proper dental hygiene as a preventive measure against serious health complications. According to the Mayo Clinic, poor oral health can lead to significant conditions such as endocarditis, cardiovascular disease, pregnancy complications, and pneumonia. Consequently, effective dental hygiene education and preventive care can provide substantial health benefits that extend well beyond oral health alone.
Recognizing the multifaceted benefits of accessible oral healthcare, Marshfield has partnered with Smiles on Wheels to offer monthly dental services—including cleanings, sealants, and fluoride treatments—at their primary care clinic, regardless of insurance. This initiative has been especially beneficial for young children and parents who face financial challenges related to transportation, and helps Marshfield to more effectively ensure high-value care for all patients. It also helps families avoid future costs associated with more complex treatments that may result from a lack of preventive care. The program has received positive feedback from the patient population, with many community members expressing their gratitude for the support it provides.
Figure 1. Smiles on Wheels provides dental care services to Marshfield Medical Center-Dickinson patients during wellness care visits.
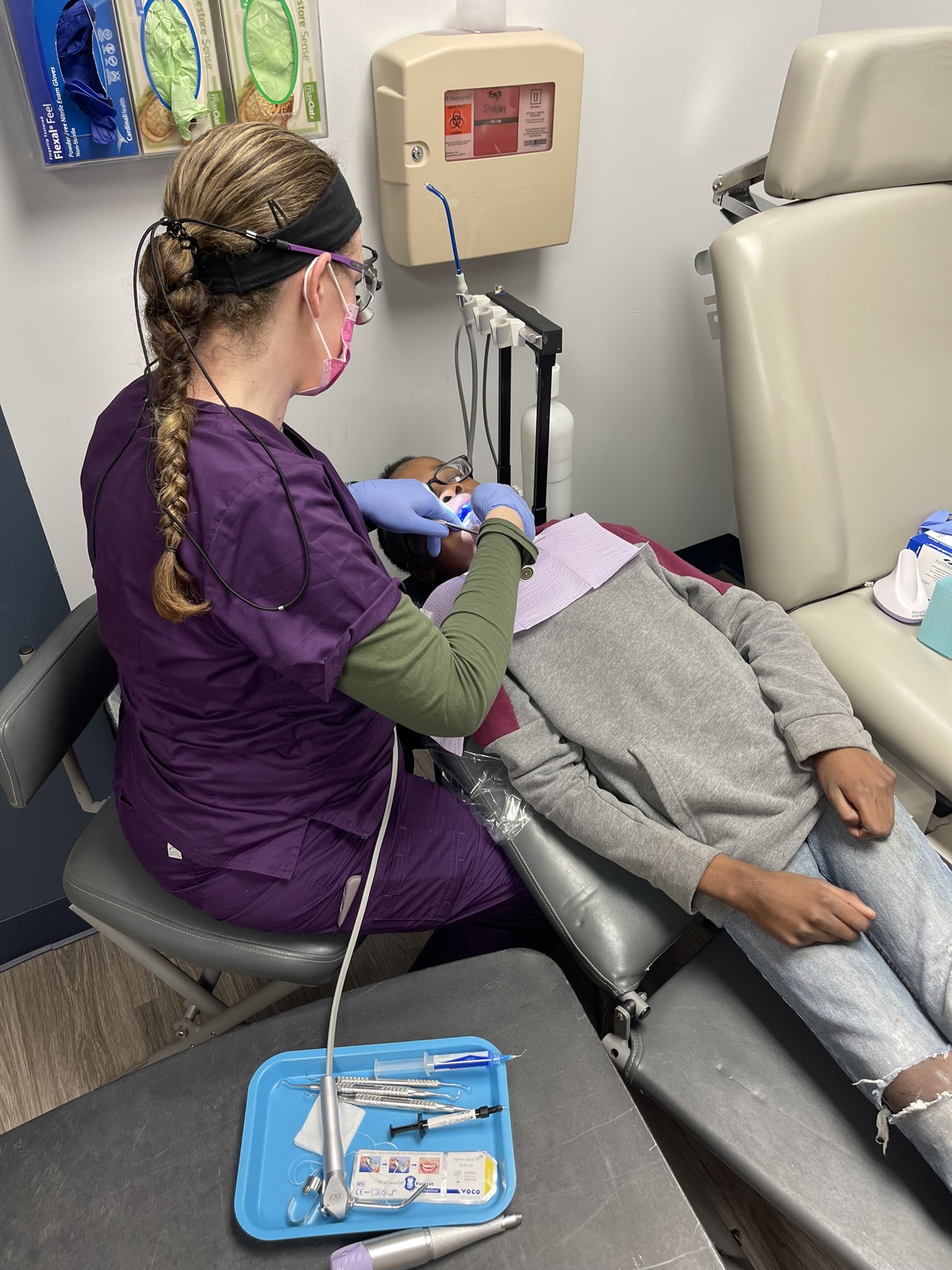
Photo courtesy of Marshfield Medical Center-Dickinson
Dr. Alexis Cirilli Whaley, MMC-D Pediatrician said, “We are fortunate to have Smiles on Wheels offering dental care to our local children, particularly for those families needing additional support due to economic stressors. The initiative allows for increased access to dental treatment, conveniently scheduled during wellness care visits."
By partnering with Smiles on Wheels, Marshfield Medical Center-Dickinson is leveraging existing resources to create a meaningful impact. This collaboration optimizes the use of available assets and showcases an effective strategy that harnesses the strengths of community partners. Stories like that of Marshfield Medical Center-Dickinson highlight the power of community partnerships in bridging known gaps in care and making a significant difference.
If your hospital or organization has an initiative they would like to share, please contact the Coordinating Center at Michigan-Value-Collaborative@med.umich.edu – we would love to hear from you.