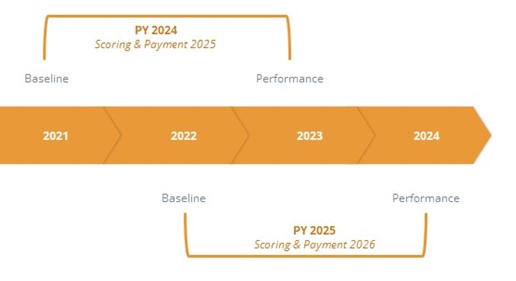
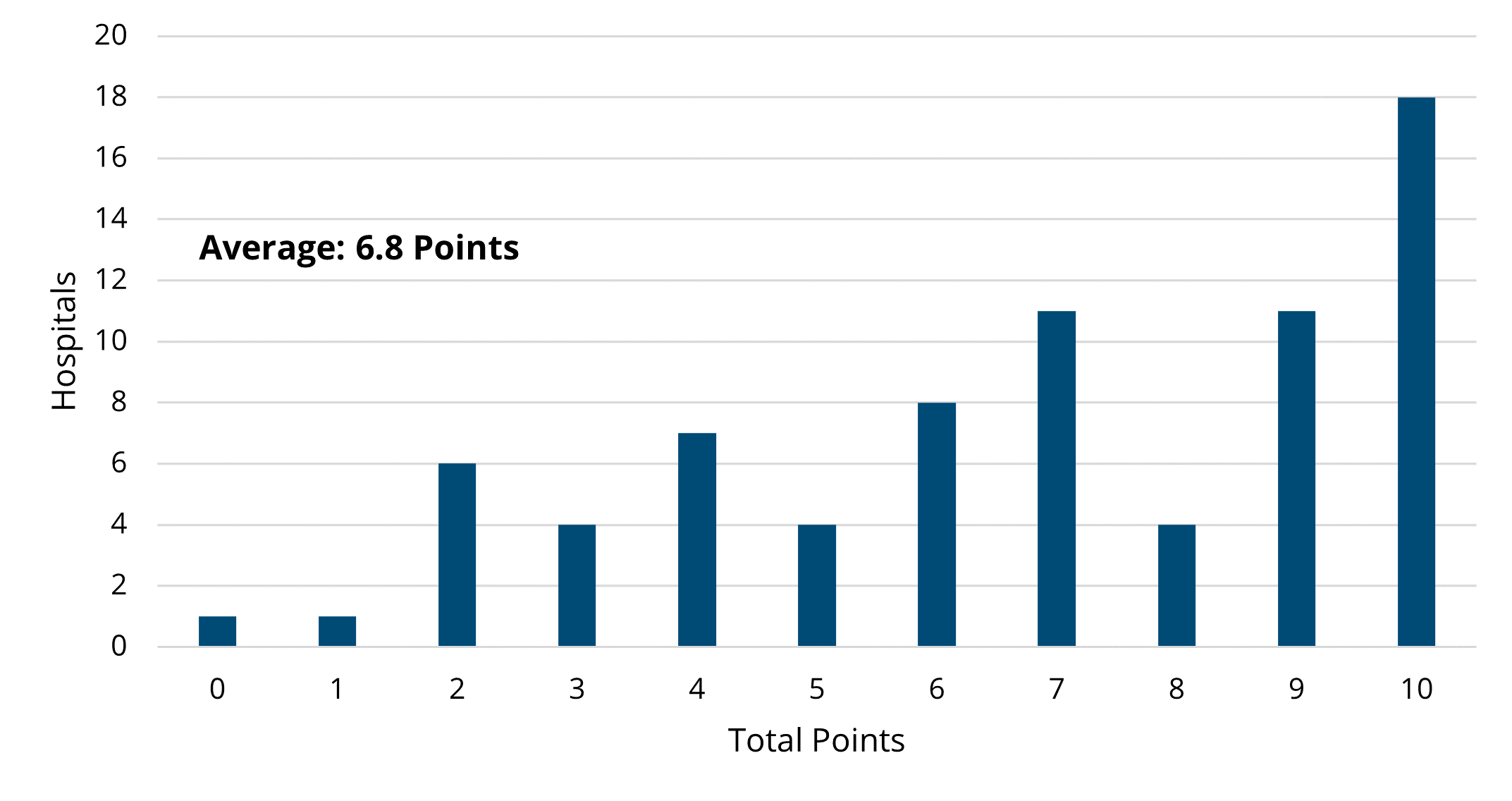The Michigan Value Collaborative (MVC) Coordinating Center distributed final scorecards for Program Year (PY) 2024 of the MVC Component of the Blue Cross Blue Shield of Michigan (BCBSM) Pay-for-Performance (P4P) Program. This report provided hospitals with their final score for PY 2024 as well as detailed breakdowns by scoring component. This was the first year of a two-year cycle for which MVC claims data was used to score hospitals on their episode spending and value metric selections. PY 2024 used baseline year claims data from 2021 and performance year data from 2023.
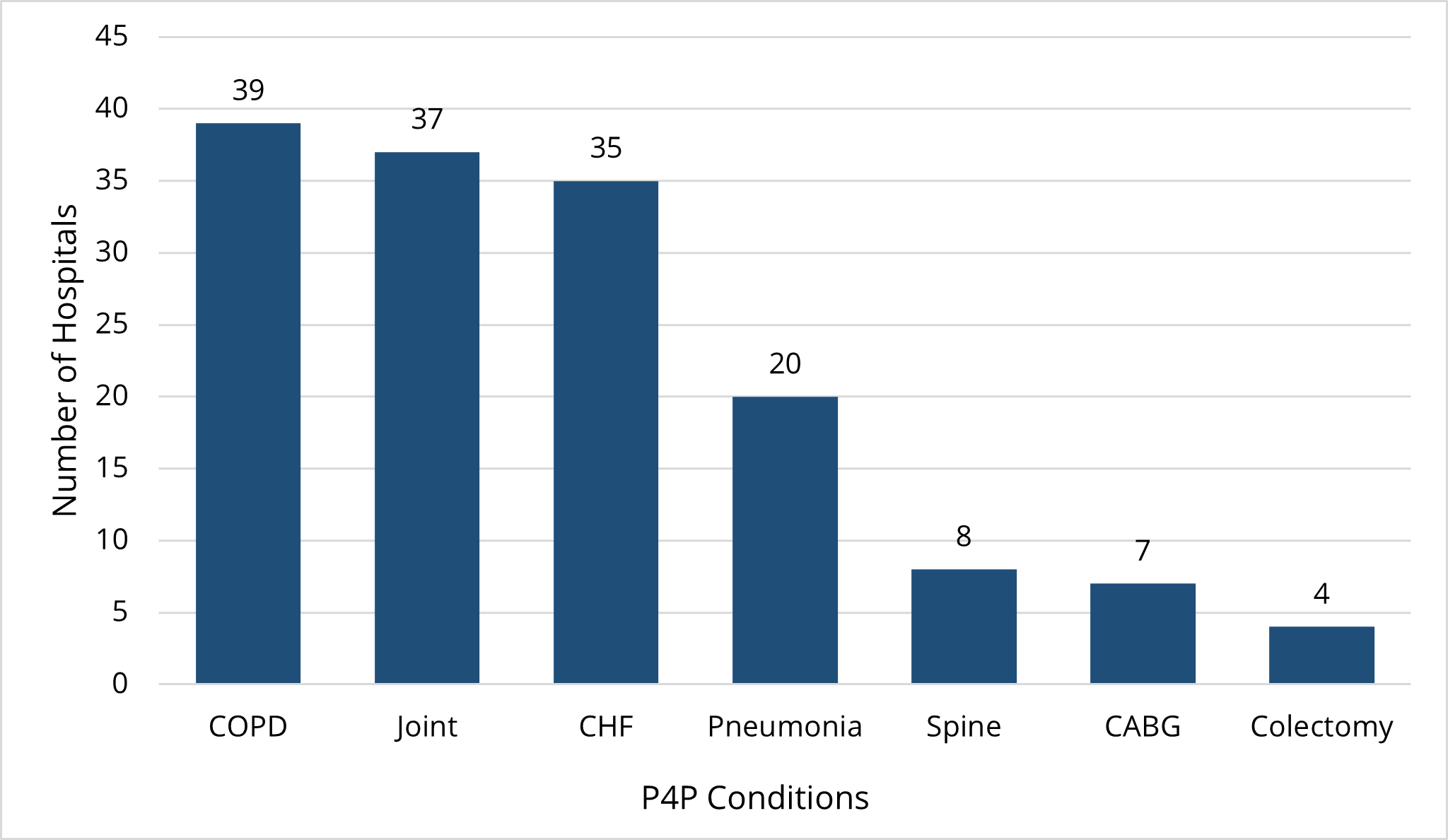
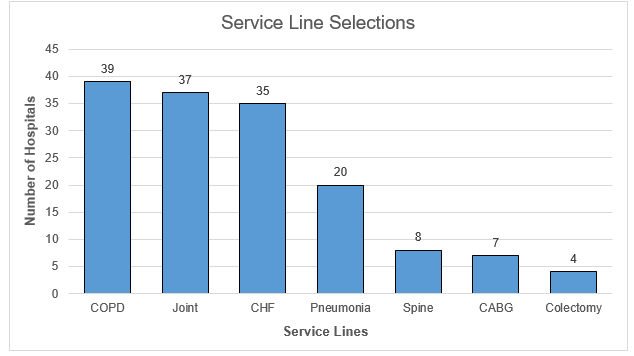
The episode spending conditions for which MVC is scoring hospitals for PY 2024 include chronic obstructive pulmonary disease (COPD), colectomy (non-cancer), congestive heart failure (CHF), coronary artery bypass graft (CABG), joint replacement (hip and knee), and pneumonia. These conditions differ slightly from the list of episode spending conditions available in the PY 2026-2027 cycle (view PY 2026-2027 FAQ). Figure 1 shows the frequency of hospital selections for the PY 2024-2025 program cycle for episode spending; the plurality of hospitals selected joint replacement, whereas pneumonia was selected the least.
The value metrics for which MVC scored hospitals for PY 2024 included cardiac rehabilitation after CABG, cardiac rehabilitation after percutaneous coronary intervention (PCI), follow-up after CHF, follow-up after COPD, follow-up after pneumonia, preoperative testing, and risk-adjusted readmissions after sepsis. Figure 2 shows that the plurality of hospitals selected 7-day follow up after CHF, and both 90-day cardiac rehab after CABG & 30-day inpatient readmissions after sepsis were selected the least.
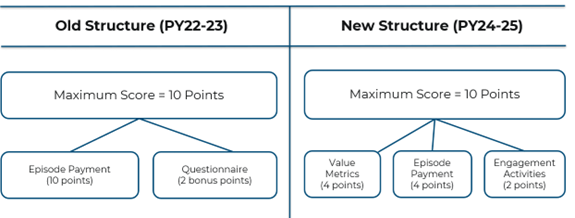
The MVC Component of the BCBSM P4P Program evaluated each participating hospital’s risk-adjusted, price-standardized, average 30-day episode payments for their selected condition as well as rates of utilization for their selected value metric through two methods. Hospitals earned points via "improvement" by reducing their payment or improving their utilization rate from the baseline period, or alternatively earned "achievement" points by being less expensive or having a better relative utilization rate than the peers in their designated cohort. The MVC cohorts are groups of hospitals determined to be peers using factors such as hospital bed size and case mix index.
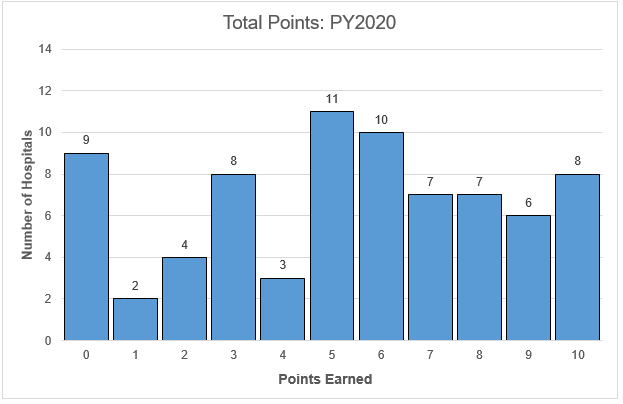
While hospitals were scored on both improvement and achievement, members received the higher of those two scores for each of their selections. Hospitals were also eligible to receive engagement points by completing eligible MVC activities. A maximum of 10 points (4 points each for the selected episode spending condition and value metric, 2 points from engagement activities) were awarded to participating members. The distribution of total points earned by hospitals for the PY 2024 is illustrated in Figure 3.
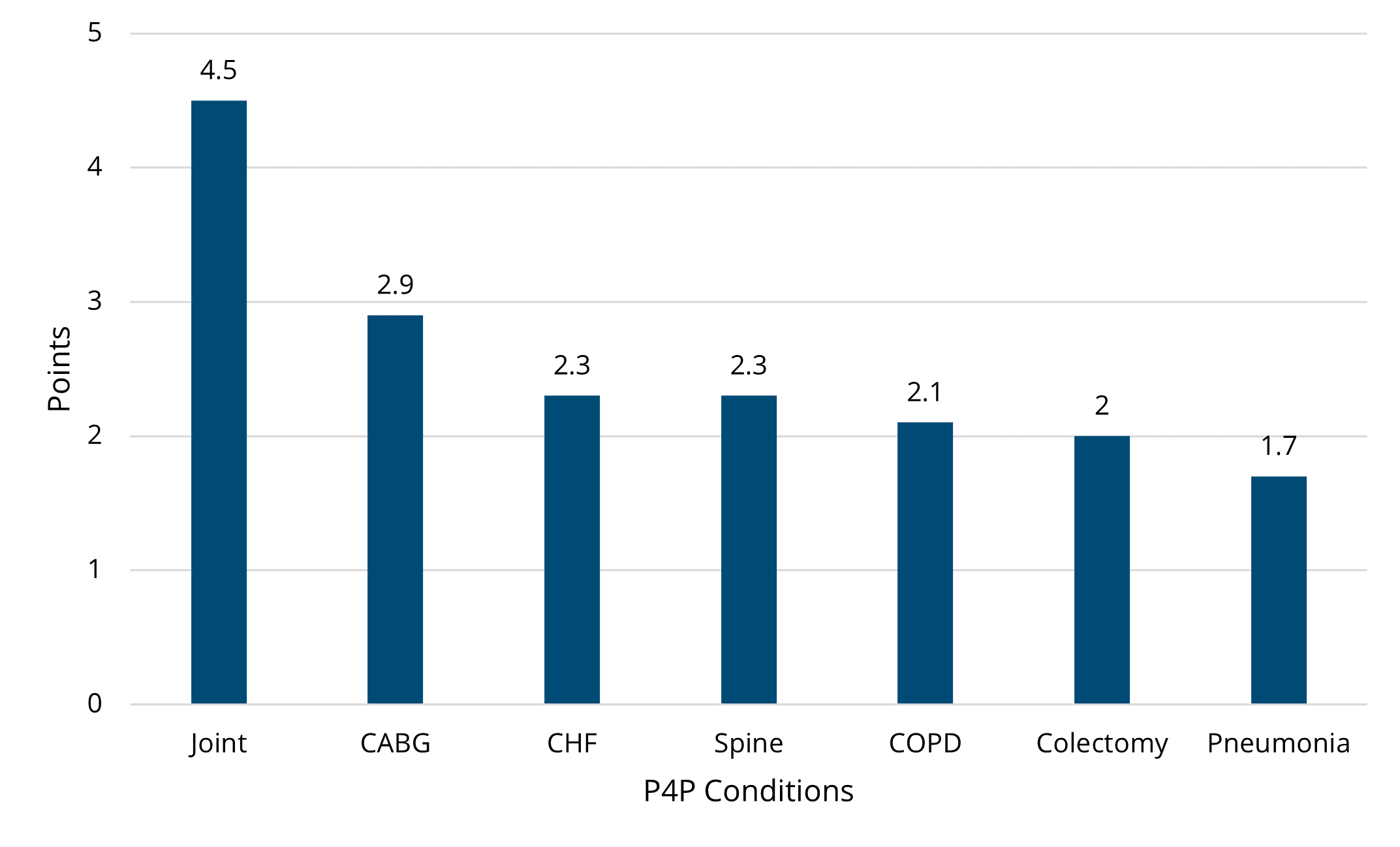
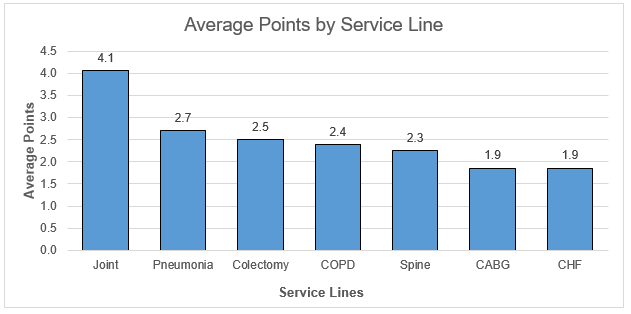
On average, hospitals earned 6.6 points in total, a decrease of 0.8 points from the PY 2023 average of 7.4 points. Figure 4 shows that the episode spending condition with the highest average awarded points was joint replacement (3.1 points) followed by CABG (2.3 points). Similarly, Figure 5 shows that the value metric with the highest average awarded points was preoperative testing (3.3 points) followed by 90-day cardiac rehabilitation after PCI (2.7 points). The breakdown of average points by each program component is illustrated in Figure 6. On average, hospitals earned 1.7 of the 2 available engagement points.
If you have any questions regarding PY 2024 of the MVC Component of the BCBSM P4P Program, please refer to the MVC P4P PY 2024-2025 Technical Document. If you would like to set up a meeting to review your hospital’s program year selections or scores, please contact the Coordination Center [EMAIL]. MVC will evaluate and release mid-year scorecards for PY 2025 in the summer of 2025.