Non-adherence to a prescribed medication regime for chronic disease management is known to lead to poor health outcomes and higher healthcare costs. A number of studies have shown that adherence is usually around 50% or less, even when medications are provided free of charge. What seems to be less clear is how best to address poor adherence; one study points out that most of the current interventions meant to improve adherence rates are too complex or ineffective, and that the research in this field is rife with weaknesses and bias.
But as with most quality improvement initiatives, understanding the source of the problem is an important first step. In this case, identifying the reasons for non-adherence is an important starting point for reducing barriers and improving patient outcomes. Many factors may affect whether a person takes their medications, including the patient themselves, the disease being treated, the health system and team, and the type of therapy involved. One study’s survey of 10,000 patients found that the most cited barrier to taking one’s medications was simply forgetfulness (24%). This was followed by perceived side effects (20%), high drug costs (17%), and a perception that their prescribed medication will have very little effect on their disease (14%).
The same study illustrated the various patient, provider, and external factors that can play a role in medication adherence using the figure below (Figure 1). If any one of these factors were to present a challenge for the patient, then they are at risk of not taking their prescribed medications on time and any related medical issues.
Figure 1.
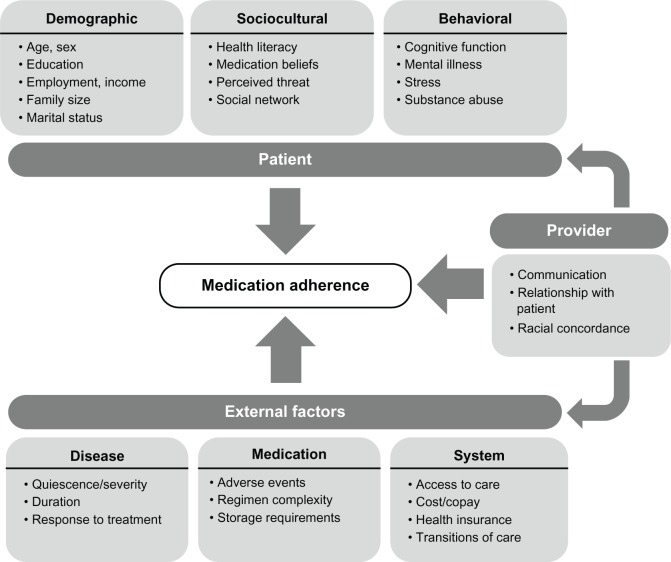
While some interventions such as pill box aids and electronic reminders have helped patients when forgetfulness is the issue, these do not address factors such as concerns about side effects and medication-related harm, or uncertainty about the importance of taking long-term prescribed medications. These issues have the potential to be addressed through shared decision-making and education from clinical experts such as pharmacists and nurses.
One review analyzed the impact that social determinants of health has on medication adherence. Disadvantageous circumstances in social and living conditions are associated with an increase in chronic disease, and it is believed that these same challenges impact a person’s ability to manage their health. When an individual is facing food insecurity, unemployment, and unstable living conditions, they are sometimes unable to address their health concerns emotionally or financially. The review found that medication adherence was negatively impacted by food insecurity and housing instability, although few studies identified other specific social determinants that influence non-adherence to medications beyond these two. In fact, education, income, and employment status did not significantly correlate with adherence to a medication regime.
The Michigan Value Collaborative (MVC) would like to hear how your institution is addressing medication non-adherence, especially in the chronic disease patient population. This will be an upcoming topic at a chronic disease management workgroup. Please contact MVC at michiganvaluecollaborative@gmail.com for information about attending.



