This week the Michigan Value Collaborative (MVC) Coordinating Center announced the condition selection process for program year (PY) 2022 and PY 2023 of the MVC Component of the Blue Cross Blue Shield of Michigan (BCBSM) Pay-for-Performance (P4P) program. The timeline for each program year’s stages are detailed in Figure 1.
Figure 1.
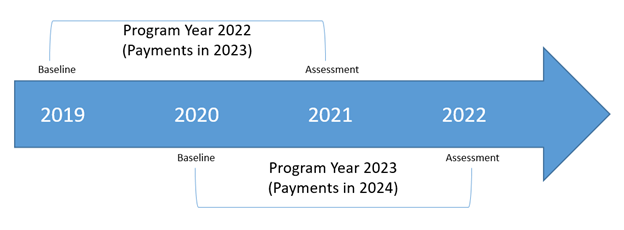
In the announcement, hospitals were tasked with selecting two conditions for which they will be evaluated and returning their condition selection form to the Coordinating Center by Friday, August 13, 2021. The announcement also outlined changes to the scoring methodology, cohort assignments, and bonus points available.
The Coordinating Center’s recent announcement included condition selection reports with targets for each condition option that may help inform hospitals’ selection decisions. Each participating hospital will choose two of the seven available conditions for PY22 and PY23: spine surgery, joint replacement, chronic obstructive pulmonary disease (COPD), coronary artery bypass grafting (CABG), congestive heart failure (CHF), colectomy (non-cancer), and pneumonia. When selecting conditions, the Coordinating Center recommends reviewing your data in the registry and considering several factors for each condition, including case counts and identifiable areas with the greatest cost opportunities. The Coordinating Center also recommends considering where resources are currently being directed in your facility and potentially aligning with those efforts.
One notable change from prior program years is the methodology by which hospitals earn achievement and improvement points. Hospital scores will continue to be based on a hospital’s risk-adjusted, price-standardized total episode payments for two selected conditions, and they can still earn a maximum score of 10 points. However, the improvement and achievement scores will become more similar in order to be placed on the same scale. As such, the achievement equation will change from being based on rank within MVC cohort at performance year to being based on distance from MVC cohort mean at baseline year. Similarly, the improvement equation will utilize the distance from the hospital’s mean at baseline. These new equations (see Figure 2) as well as complete descriptions of the updated methodologies are reviewed at length with examples in the technical document.
Figure 2.

P4P cohorts have also been reassigned for PY22 and PY23. These changes are also detailed in the technical document, and the new cohort assignments can be found on the MVC website. The cohorts are not intended to group hospitals that are exactly alike; rather, they create a reasonably-comparable grouping from which MVC can complete statistical analysis.
The final change is to the awarding of bonus points. In place of the previous 5% cohort reduction bonus, participants can instead earn bonus points by completing two questionnaires (one per selected condition) and submitting these to the Coordinating Center by November 1st of each program year. The purpose of this is to gather examples of quality improvement initiatives in operation at MVC member hospitals to share with the Collaborative. Moving forward, this will help support members in reducing costs through collaboration.
Each of the changes mentioned above are designed to deliver a more transparent, intuitive, flexible, and fairer P4P program. The Coordinating Center will offer an explainer webinar to answer questions and walk through the details of these changes in more detail. The webinar will be offered on two dates: the first is scheduled for Thursday, July 29 from 11:00-12:00 pm, and the second is on Tuesday, August 3 from 1:00-2:00 pm. Both webinars can be accessed using the following Zoom link: https://umich.zoom.us/j/95502303999. Participants can also call +1 301 715 8592 (meeting ID #955 0230 3999). For those interested in the explainer webinar who are unavailable on both dates, a recording of the first webinar will be available. If you are interested in receiving a link to this recording, please email the MVC team at michiganvaluecollaborative@gmail.com.